- Large motor delays
- Failure to thrive, growth delays
- Low muscle tone
- Extreme fatigue
- Inability to regulate temperature
- Autistic symptoms
- Global muscle weakness
- Difficulty waking
Even if your child does not display any of the “classic” symptoms of mitochondrial dysfunction (listed above), your child may still be affected.
It is now believed by many research scientists and an increasing number of physicians that mitochondrial dysfunction may be a critical part of the underlying pathophysiology in the following health conditions:
- Parkinson’s disease
- Asthma
- Chronic fatigue syndrome
- Alzheimer’s disease
- Some gastronintestinal disorders, among others
What Is Mitochondrial Dysfunction?
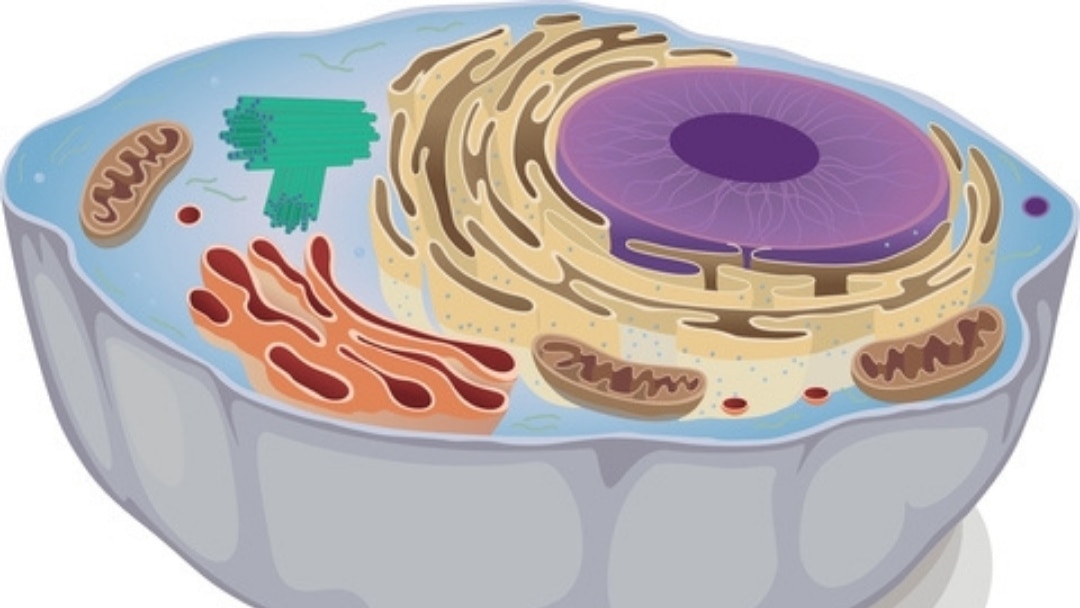
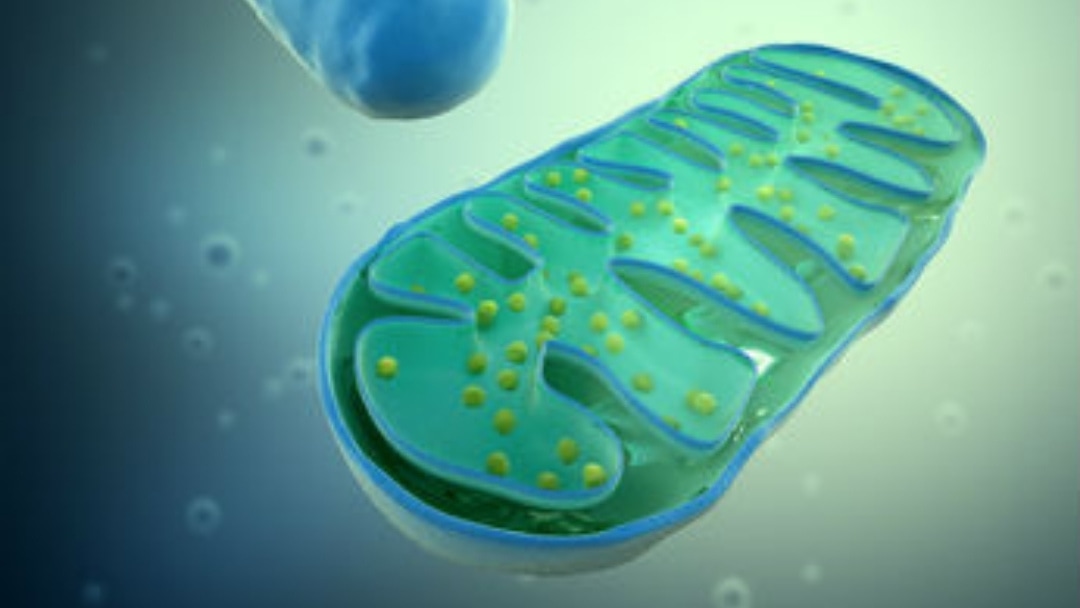
Mitochondria are the “power plants” of the body. They make the energy to power cells in every part of the body, including the major organs requiring significant amounts of energy to function properly. The organs in the body that require the most energy are the brain, muscles, liver, kidneys, gastrointestinal tract, heart and lungs.
Mitochondrial disease or mitochondrial dysfunction is what occurs when the mitochondria are not able to do their job due to genetic or environmental factors. When the mitochondria are not working properly, a whole host of symptoms may appear. According to the UMDF (United Mitochondrial Disease Foundation), an affected individual may have:
- Strokes
- Seizures
- Gastrointestinal problems (reflux, vomiting, constipation, diarrhea)
- Swallowing difficulties
- Failure to thrive
- Blindness
- Deafness
- Heart and kidney problems
- Muscle failure
- Heat/cold intolerance
- Diabetes
- Lactic acidosis
- Immune system problems
- Liver disease
An undiagnosed child may exhibit feeding problems, be unable to fight typical childhood infections or have repeated infections and fevers without a known origin. A red flag for mitochondrial dysfunction is when a child has more than three organ systems with problems or when a typical disease exhibits atypical qualities.
How Do I Know If My Child Has Mitochondrial Dysfunction?
There are certain blood tests that may indicate that a child has mitochondrial dysfunction. Ask an integrative or holistic physician or practitioner to look for the following “red flags” in laboratory blood work:
- Elevated levels of:
- Ammonia
- Alanine
- Alanine/lysine ratio
- Glycine
- Proline
- Tyrosine
- Sarcosine
- Lactate/pyruvate ratio
- Acetyl free carnitine ratio
- Elevations suggesting disruptions in fatty acid oxidation
- Reduced free and total carnitine
- Irregular urine organic acid screening:
- TCA intermediates
- Ehylmalonate
- 3-methylglutaconate
- Dicarboxylic acids
- Methylmalonic acid
Consider seeing a geneticist who specializes in mitochondrial disease. A list of mitochondrial disease doctors/specialists (with hospital affiliation) can be found here.
A Mitochondrial Dysfunction Healing Checklist
Exercise:
Exercise helps the body’s mitochondria make new, baby mitochondria, so even though your child may loathe exercise, be sure to have them move as much as possible.
Use mitochondria-boosting supplements with your practitioner’s guidance:
- Cod liver oil
- Vitamin E
- CoQ10
- Phosphatidylcholine
- MCT coconut oil
- Acetyl-l-carnitine
Still Looking for Answers?
Visit the Epidemic Answers Practitioner Directory to find a practitioner near you.
Join us inside our online membership community for parents, Healing Together, where you’ll find even more healing resources, expert guidance, and a community to support you every step of your child’s healing journey.
Join MitoAction every 2nd Tuesday of the month at 12:30 EST to participate in a discussion regarding mitochondrial dysfunction and autism. Call in to the conference call by phoning 1-866-414-2828 and enter code 017921# at the prompt.
Sources & References
Andreazza, A.C., et al. Mitochondrial complex I activity and oxidative damage to mitochondrial proteins in the prefrontal cortex of patients with bipolar disorder. Arch Gen Psychiatry. 2010 Apr;67(4):360-8.
Balcells, Cristy. Autism & Mitochondrial Disorders: How Much Do We Really Know?. MitoAction.org. 29 Jan 2009
Beal, M.F., et al. Therapeutic approaches to mitochondrial dysfunction in Parkinson’s disease. Parkinsonism Relat Disord. 2009 Dec;15 Suppl 3:S189-94.
Bradford, B.L., et al. Mitochondrial Dysfunction and Type 2 Diabetes. Science. 2005 Jan 21;307(5708):384-7.
Bradstreet, J.J., et al. Biomarker-guided interventions of clinically relevant conditions associated with autism spectrum disorders and attention deficit hyperactivity disorder. Altern Med Rev. 2010 Apr;15(1):15-32.
Burchell, V.S., et al. Targeting mitochondrial dysfunction in neurodegenerative disease: Part I. Expert Opin Ther Targets. 2010 Apr;14(4):369-85.
Burchell, V.S., et al. Targeting mitochondrial dysfunction in neurodegenerative disease: Part II. Expert Opin Ther Targets. 2010 May;14(5):497-511.
Davi, Alyssa. Has Your Child with Autistic Symptoms Been Properly Screened for a Subset of Mitochondrial Disease Known as OXPHOS?…Probably Not. Autism File. 2010; 36.
Dehley, Leanna M., et al. The Effect of Mitochondrial Supplements on Mitochondrial Activity in Children with Autism Spectrum Disorder. J Clin Med. 2017 Feb; 6(2): 18.
Ferrer, et al. Early involvement of the cerebral cortex in Parkinson’s disease: convergence of multiple metabolic defects. Prog Neurobiol. 2009 Jun;88(2):89-103.
Filipek, P.A., et al. Relative carnitine deficiency in autism. J Autism Dev Disord. 2004 Dec;34(6):615-23.
Haas, R.H., et al. Mitochondrial disease: a practical approach for primary care physicians. Pediatrics. 2007 Dec;120(6):1326-33.
Hao, J., et al. Mitochondrial nutrients improve immune dysfunction in the type 2 diabetic Goto-Kakizaki rats. J Cell Mol Med. 2009 Apr;13(4):701-11.
Herbert, M.R. Contributions of the environment and environmentally vulnerable physiology to autism spectrum disorders. Curr Opin Neurol. 2010 Apr;23(2):103-10
James, S.J., et al. Cellular and mitochondrial glutathione redox imbalance in lymphoblastoid cells derived from children with autism. FASEB J. 2009 Aug;23(8):2374-83.
Kato, T. The role of mitochondrial dysfunction in bipolar disorder. Drug News Perspect. 2006 Dec;19(10):597-602.
Kelley, R.I. Evaluation and Treatment of Patients with Autism and Mitochondrial Disease. Kennedy Krieger Institute, Division of Metabolism.
Klehm, M., et al. Clinician’s Guide to the Management of Mitochondrial Disease: A Manual for Primary Care Providers. MitiAction.org. 2014.
Konradi, C., et al. Molecular evidence for mitochondrial dysfunction in bipolar disorder. Arch Gen Psychiatry. 2004 Mar;61(3):300-8.
Korson, M. Mitochondrial Disease and Patient Challenges. MitoAction. 2008.
Leib, S., et al. Mitochondrial Oxidative Phosphorylation (OXPHOS) Dysfunction: A Newly Emerging Category of Autistic Spectrum Disorder Information for Primary Care Physicians. MitoAction.org. 2010.
Liu, J. The effects and mechanisms of mitochondrial nutrient alpha-lipoic acid on improving age-associated mitochondrial and cognitive dysfunction: an overview. Neurochem Res. 2008 Jan;33(1):194-203.
Long, J., et al. Mitochondrial decay in the of old rats: ameliorating effect of alpha-lipoic acid and acetyl-L-carnitine. Neurochem Res. 2009 Apr;34(4):755-63.
Mabalirajan, U., et al. Effects of vitamin E on mitochondrial and asthma features in an experimental allergic murine model. J Appl Physiol. 2009 Oct;107(4):1285-92.
Maes, M., et al. Coenzyme Q10 deficiency in myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) is related to fatigue, autonomic and neurocognitive symptoms and is another risk factor explaining the early mortality in ME/CFS due to cardiovascular disorder. Neuro Endocrinol Lett. 2009;30(4):470-6.
Maes, M., et al. Lower plasma Coenzyme Q10 in depression: a marker for treatment resistance and chronic fatigue in depression and a risk factor to cardiovascular disorder in that illness. Neuro Endocrinol Lett. 2009;30(4):462-9.
Morino, K., et al. Molecular mechanisms of insulin resistance in humans and their potential links with mitochondrial dysfunction. Diabetes. 2006 Dec;55 Suppl 2:S9-S15.
Noland, R.C., et al. Carnitine insufficiency caused by aging and overnutrition compromises mitochondrial performance and metabolic control. J Biol Chem. 2009 Aug 21;284(34):22840-52.
Oliveira, G., et al. Mitochondrial dysfunction in autism spectrum disorders: a population-based study. Dev Med Child Neurol. 2005 Mar;47(3):185-9.
Palmieri, L., et al. Mitochondrial dysfunction in autism spectrum disorders: cause or effect? Biochim Biophys Acta. 2010 Jun-Jul;1797(6-7):1130-7.
Parikh, S. The neurologic manifestations of mitochondrial disease. Dev Disabil Res Rev. 2010;16(2):120-8.
Parikh, S., et al. A Modern Approach to the Treatment of Mitochondrial Disease. Current Treatment Options in Neurology. 2009 Nov;11(6):414-30.
Pastural, E., et al. Novel plasma phospholipid biomarkers of autism: mitochondrial dysfunction as a putative causative mechanism. Prostaglandins Leukot Essent Fatty Acids. 2009 Oct;81(4):253-64.
Power, R.A., et al. Carnitine revisited: potential use as adjunctive treatment in diabetes. Diabetologia. 2007 Apr;50(4):824-32.
Rector, R.S., et al. Mitochondrial dysfunction precedes insulin resistance and hepatic steatosis and contributes to the natural history of non-alcoholic fatty liver disease in an obese rodent model. J Hepatol. 2010 May;52(5):727-36.
Schmidt, Charles W. Mito-Conundrum: Unraveling Environmental Effects on Mitochondria. Environmental Health Perspectives. 2010 July; 118(7).
Scirocco, A., et al. Exposure of Toll-like receptors 4 to bacterial lipopolysaccharide (LPS) impairs human colonic smooth muscle cell function. J Cell Physiol. 2010 May;223(2):442-50.
Shen, W., et al. Protective effects of R-alpha-lipoic acid and acetyl-L-carnitine in MIN6 and isolated rat islet cells chronically exposed to oleic acid. J Cell Biochem. 2008 Jul 1;104(4):1232-43.
Shekhawat, P.S., et al. Spontaneous development of intestinal and colonic atrophy and inflammation in the carnitine-deficient jvs (OCTN2(-/-)) mice. Mol Genet Metab. 2007 Dec;92(4):315-24.
Shoffner, J., et al. Fever Plus Mitochondrial Disease Could Be Risk Factors for Autistic Regression. J Child Neurol. 2010 Apr;25(4):429-34.
Shokolenko, I., et al. Oxidative stress induces degradation of mitochondrial DNA. Nucleic Acids Res. 2009 May; 37(8): 2539–2548.
Sifroni, K.G., et al. Mitochondrial respiratory chain in the colonic mucosal of patients with ulcerative colitis. Mol Cell Biochem. 2010 Sep;342(1-2):111-5.
Spindler, M., et al. Coenzyme Q10 effects in neurodegenerative disease. Neuropsychiatr Dis Treat. 2009;5:597-610.
Sreekumar, R., et al. Skeletal muscle mitochondrial dysfunction & diabetes. Indian J Med Res. 2007 Mar;125(3):399-410.
Taurines, R., et al. Expression analyses of the mitochondrial complex I 75-kDa subunit in early onset schizophrenia and autism spectrum disorder: increased levels as a potential biomarker for early onset schizophrenia. Eur Child Adolesc Psychiatry. 2010 May;19(5):441-8.
Weissman, J.R., et al. Mitochondrial Disease in Autism Spectrum Disorder Patients: A Cohort Analysis. PLoS One. 2008;3(11):e3815.
Zhang, H., et al. Combined R–alpha-lipoic acid and acetyl-L-carnitine exerts efficient preventative effects in a cellular model of Parkinson’s disease. J Cell Mol Med. 2010 Jan;14(1-2):215-25.