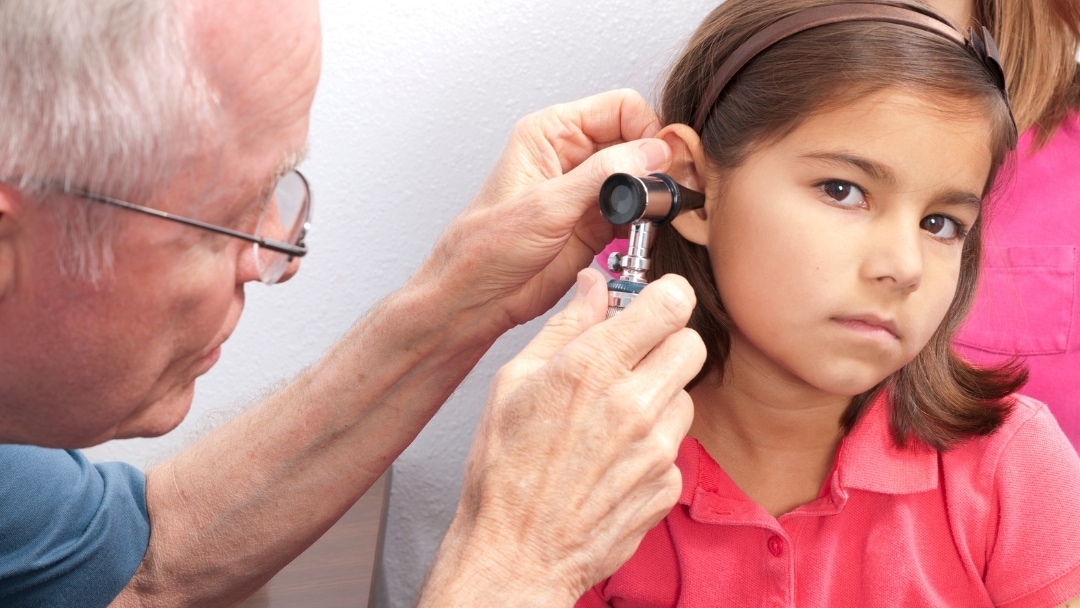
Kelly Dorfman MS LND discusses the relationship between ear infections and autism in this post.
Many years ago, a group of parents and professionals discussed concerns about the emergence of a regressive autistic-like syndrome, later named Pervasive Developmental Disorder (PDD), which is on the autism spectrum. All knew children whose development regressed following frequent otitis media (inner ear infections). Could ear infections and autism and/or PDD be linked?
The autism epidemic now claims an estimated one in 36 children.
Some experts suspect the mercury-based preservative thimerosal as a major culprit, but one factor alone is not responsible for PDD or autism; instead, the total load of stressors must be considered. Ear infections remain shadowy contributors.
Perhaps a subgroup of children on the autistic spectrum, including those with attention deficits and learning disabilities, have a condition named Post-Traumatic Ear Infection Syndrome (PTEIS). These kids are apparently normal at birth, develop continuous ear infections and subsequent auditory processing issues and developmental delays as a result of complications from sustained damage to the inner ear from both the disease and its treatment.
Why Are Ear Infections Such a Problem?
Frequent ear infections are a sign of weak immune function.
Most children on the autism spectrum have underlying immune problems. Either they are born with weak immunity, making them more reactive to foods, or they react to foods, thus weakening their immune systems.
Resultant ear infections are the symptom of a deeper underlying problem. A classic study done by Talal Nsouli found that 78% of children with otitis media have food allergies. When the offending foods were removed from the diet, 86% of ear infections subsided. Upon challenge with offending foods, 94% of children had a recurrence of ear infection.
Kids with food allergies get sick more often because their immune systems focus on reacting to foods, rather than on fighting germs.
Antibiotics used to treat ear infections may make children more susceptible to damage from mercury and other toxins.
Preliminary studies by Dr. Boyd Haley, the world authority on mercury, found that the antibiotics ampicillin and tetracycline increase thimerosal-induced neuronal death. In other words, less mercury does more damage in the presence of these antibiotics. In addition, a meta-analsyis showed that the vast majority (74%) of studies suggest that mercury is a risk factor for autism, revealing both direct and indirect effects. Mercury exposure typically comes from the thimerasol preservative as well as mother-to-child transmission, especially from a mother who has mercury amalgams (“silver fillings”).
Furthermore, all antibiotics kill good gut bacteria, which are essential to resist mercury uptake. Allergies, food sensitivities, ear infections, thimerosal and antibiotics are a potent cocktail for autism.
A child eats an allergic food and develops an ear infection. The doctor prescribes an antibiotic, killing both good and bad bacteria, leaving the gut lining irritated and in a state of gut dysbiosis, further stimulating an allergic response. Now the child is more reactive to foods, and develops additional ear infections, thus perpetuating an illness cycle.
Introduce into this disturbing spiral thimerosal. Who will be more likely to sustain the damage, the toddler with an already irritated gut lining and reactive immune system, or a healthy child? Children with autism have a significantly increased rate of ear infections.
Ear infections are associated with auditory processing problems.
Children are born with hearing but they must learn how to listen. Ear infections that occur during critical developmental milestones periods negatively affect auditory processing. Children whose ears are clogged up with fluid cannot interact appropriately with their environments.
Between birth and three children learn to distinguish sounds and interpret them in context. They must filter out unimportant sounds such as the air conditioning, and focus on important ones, such as their mother’s voice.
Distracted and inattentive behavior can be the result of the inability to sort significant auditory input from the extraneous. Students who are more distracted than their peers often experienced early ear infections.
What To Do About Ear Infections
Remove problematic foods
The four problem foods most associated with ear infections are milk-based products, wheat, soy and eggs. Before trying an elimination diet, consider taking foods made from cow’s milk out of the diet first. This change alone is often sufficient to reduce or stop infections.
Use good bacteria
Probiotics, available in the refrigerator section of health food stores, balance the digestive tract and reduce allergic tendencies. It may take some trial and error to find the right product for your individual situation. Some are too strong and will increase gas and irritability; others are not potent enough. If symptoms do not alleviate in a few days, reduce the dose or change brands.
Final thoughts
PTEIS is very common and mostly preventable. If you have a child who has had three or more ear infections, do not wait. We have learned the importance of taking preventive action. For more information read Schmidt’s Healing Childhood Ear Infections and McCandless’ Children with Starving Brains.
About Kelly Dorfman MS LND
Kelly Dorfman is one of the world’s foremost experts on using nutrition therapeutically to improve brain function, energy and mood. Kelly’s special talent for integrating information from many sources and finding practical solutions has made her a popular speaker and workshop leader. She lectures extensively and is a member of Platform (formerly the National Speakers Association) and has been featured on numerous television programs including CNN’s American Morning.
Kelly’s award winning book, Cure Your Child With Food: The Hidden Connection Between Nutrition and Childhood Ailments (formerly known as What’s Eating Your Child) was given rave reviews by Publishers Weekly and the Washington Post.

As a go-to expert on nutrition issues, Kelly is frequently interviewed and quoted in the media. She has been featured in articles in The Wall Street Journal, Parade, Bethesda magazine, Living Without magazine, and the Huffington Post.
Kelly holds a master’s degree in nutrition/biology and is a licensed nutrition dietitian. She is a co-founder of Developmental Delay Resources, which has merged with Epidemic Answers. You can find out more about Kelly and her practice at kellydorfman.com
Still Looking for Answers?
Visit the Epidemic Answers Practitioner Directory to find a practitioner near you.
Join us inside our online membership community for parents, Healing Together, where you’ll find even more healing resources, expert guidance, and a community to support you every step of your child’s healing journey.
Sources & References
Adams, J.D., et al. Otitis Media and Related Complications Among Children with Autism Spectrum Disorders. J Autism Dev Disord. 2016 May;46(5):1636-42.
Bradstreet, J., et al. A Case-Control Study of Mercury Burden in Children with Autistic Spectrum Disorders. Journal of American Physicians and Surgeons. 2003 Jun;76-79.
Frieri, M. Asthma linked with rhinosinusitis: An extensive review. Allergy Rhinol (Providence). 2014;5(1):41-9.
Kern, J.K., et al. The relationship between mercury and autism: A comprehensive review and discussion. J Trace Elem Med Biol. 2016 Sep;37:8-24.
Konstantareas, M.M., et al. Ear infections in autistic and normal children. Journal of Autism and Developmental Disorders. 1987 Dec;17(4):585-94.
Nsouli, T.M., et al. The role of food allergy in serious otitis media. Ann Allergy. 1994 Sep; 66:91.
Resources
Arizona State University Autism/Asperger’s Research Program Autism-Related Scientific Articles
Books
Neustaedter, Randall. The Holistic Baby Guide: Alternative Care for Common Health Problems. New Harbinger Publications, 2010.
Schmidt, Michael. Healing Childhood Ear Infections. 1996